Telehealth: the growth and necessity of telenutrition

The demand for telehealth services has seen tremendous growth over the last few years. Yet, telehealth has become essential with COVID-19’s direct impact on the safety of patients and healthcare practitioners (HCPs) when partaking in day-to-day consultations.
The telehealth industry has also seen vast growth, with an increase in the number of platforms, functionalities and levels of integrations of electronic health records (EHR) and other technical systems supporting health care.
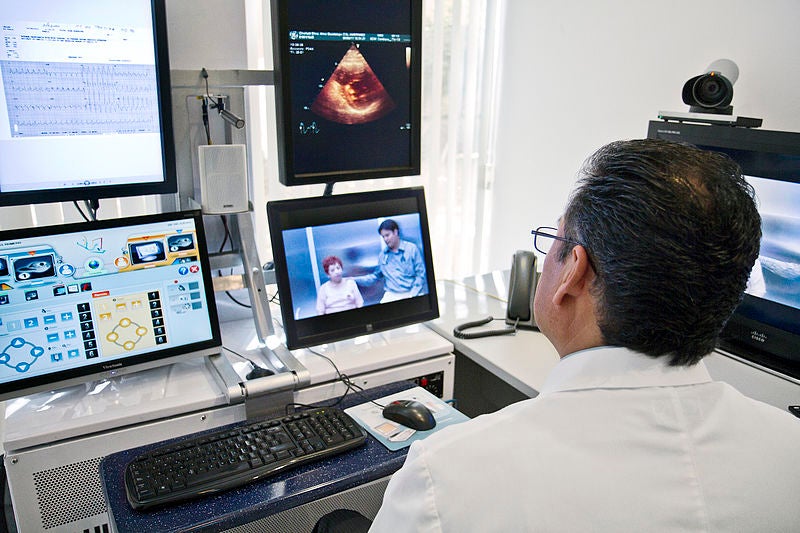
What is telehealth?
Telehealth is defined by the World Health Organisation (WHO) as the “delivery of healthcare services, where patients and providers are separated by distance”. Telehealth is also often referred to as e-Health (electronic-health) or m-Health (mobile-health).2
Telemedicine, however, is considered the application of technology when conducting clinical medicine from a distance and establishing a connection between the practitioners and patients in multiple settings.
The benefits of telehealth:
Telehealth holds multiple benefits, for both patients and HCPs. Firstly, with telehealth being “particularly valuable for those in remote areas, vulnerable groups and ageing populations”,4 it can be used when patients are unable, for any reason, to visit the HCP in person.
Secondly, “it can contribute to achieving universal health coverage by improving access for patients to quality, cost-effective, health services wherever they may be”.4
Additionally, telehealth not only benefits patients but has become incredibly useful in keeping HCPs safe from COVID-19 contraction.2 This allows for HCPs to continue practicing and helping patients, even during times of disasters or disruptions, such as a pandemic.2
Tips for HCPs using telehealth practices:
Whether you are a dietitian or pharmacist, implementing telehealth practices can be challenging for all HCPs, but there are a few tips that can help ease the process of going virtual.
The Board of Healthcare Funders (BHF) outlines some of the physical essentials when moving your consultations online :
- Stable internet connection (upload / download above 3mbps)
- Computer with webcam and integrated microphone
- Quiet & professional area in which to conduct your virtual session
- Headphones to ensure privacy
- Being professionally dressed
- Good quality lighting
What is telenutrition?
Telenutrition is a newly developing aspect of telehealth, which includes the interactive use of electronic information and telecommunications technology by a Registered Dietitian (RD), to deliver nutritional care to patients who cannot visit the RD in person.
The future of telenutrition:
Although it may come with challenges, virtual consultation in nutrition practice has been shown to be both feasible and encouraged during the COVID-19 pandemic.
For HCPs planning and building a successful therapeutic relationship with patients / clients, telenutrition may even be considered the norm in the long-term. When planning to move your practice online, Current Developments in Nutrition (CDN) recommends a set of steps.
These steps include:
- Online Presence – use social media and convert face-to-face clients into digital clients
- Preparation – setting up your environment and the clinic to connect remotely
- Connect – using the medium of choice (video-link; audio or message)
- Follow-up – ensuring continuation of care and long-term relationships with patients

Conclusion
Whether we like it or not, telehealth is on the horizon and holds many opportunities for HCPs across the world. If telehealth becomes standard practice, as is predicted, our HCPs, clinics and practices will need to begin adapting now to keep up with its evolvement.
[1]Trends in the growth of literature of telemedicine: A bibliometric analysis (Yang et al., 2015). Link: https://pubmed.ncbi.nlm.nih.gov/26415760/
[2] Global Interest in Telehealth During COVID-19 Pandemic: An Analysis of Google Trends™. (Arshad Ali, Shajeea et al., 2020) doi:10.7759/cureus.10487
[3] Clinical and Technical Considerations of an Open Access Telehealth Network in South Carolina: Definition and Deployment. (King K, Ford D, Haschker M, Harvey J, Kruis R, McElligott J., 2020). doi: 10.2196/17348
[4] Global Health Observatory (GHO) data (World Health Organisation, 2016). Link: https://www.who.int/gho/goe/telehealth/en/
[5] Telehealth for pediatric cardiology practitioners in the time of COVID-19 (Chowdhury D, Hope KD, Arthur LC, Weinberger SM, Ronai C, Johnson JN, Snyder CS, 2020). Link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7354365/
[6] COVID-19 – Guidelines: Telehealth and Telemedicine as a result of South African State of Disaster. (Board of Healthcare Funders, 2020). Link: https://www.bhfglobal.com/2020/03/27/covid-19-telehealth-telemedicine-result-south-african-state-of-disaster/
[7] The Growing Demand for Telenutrition (Cutler, 2017). Link: https://nutritioncaresystems.com/growing-demand-telenutrition/
[8] Academy of Nutrition and Dietetics, Professional resource hub: eat right pro. (2020). Link: https://www.eatrightpro.org/coronavirus-resources#telehealth-billing-coding
[9] COVID-19 and Telenutrition: Remote Consultation in Clinical Nutrition Practice, Current Developments in Nutrition, Volume 4, Issue 12 (Farid, 2020). Link: https://doi.org/10.1093/cdn/nzaa124
If you liked this post you may also like



