
Caring for Preterm and Low-Birth-Weight Infants in Resource Restricted Environments

World Prematurity Day (17 November 2021) compels the healthcare community to consider the effect of premature birth, and the burden it places on the healthcare system. “Premature birth is the leading cause of death in children under the age of five worldwide. Globally, around one million babies a year die due to complications and a lack of proper healthcare” 1. In South Africa, studies suggest that 15% of all births are premature 1.
Babies born four months premature survive in high-income counties where babies who are born two months premature die in low-income countries due to the lack of feasible and inexpensive care 2. This care refers to warmth, breastfeeding, basic hygiene to prevent infections and breathing difficulties 2.
In 2019, the global burden of deaths for children under the age of five weighed heavily in two low-income regions, being sub-Saharan Africa (2.8 million) as well as Central and Southern Asia (1.5 million). These two regions contributed just over 80% to the 5.2 million total deaths of children under the age of five 3. Causes of these deaths include infectious diseases such as pneumonia, diarrhoea, and malaria as well as preterm birth and intrapartum-related complications. Underweight children are particularly at a high risk of death from the illnesses mentioned above, due to their underdevelopment and susceptibility to illnesses 3.
To address these causes of death and prevent illness in the future, access to necessities such as childbirth-, postnatal- care, vaccinations, and early childhood preventative services is fundamental 3.
Neonatal deaths are most likely to occur in the first 28 days after birth, a third of those deaths being on the first day and almost three-quarters within the first week 3. Most of these neonatal deaths occur in countries with a low- and lower-middle- income countries, where vital services such as antenatal- , birth-, and postnatal care are lacking 3.
The good news is that simple, cost-effective interventions have demonstrated favourable outcomes in these settings. The Kangaroo Mother Care practice is a holistic process that is suitable for low-resourced countries 4,5. Breastfeeding, which is encouraged by the Kangaroo Mother Care, is reported to have excellent outcomes. Education and counselling have also been proved to assist in pregnancy outcomes and infant nutrition 7.

Kangaroo Mother Care (KMC)
KMC can be seen as a holistic and low-cost process that is suitable for both low- and high-resourced countries 4,5.
This method of care refers to the practice where an infant experiences skin-on-skin contact in an upright position with their caregiver, who acts as an incubator for the infant 4,5. Research has found that KMC is a cost-effective and high-impact practice that reduces mortality in preterm infants that weigh less than 2 000 g, and morbidity in infants 4,5. This makes KMC ideal for countries who are resource-constrained and have a high rate of premature infants, especially those in sub-Saharan Africa, which had the most neonatal deaths in 2019 3.
KMC has been linked to a 51% decrease in neonatal mortality for infants in their first week of life in comparison to incubator care 5. Although the World Health Organization (WHO) and the United Nations Children’s Fund (UNICEF) recommend that this is practiced in a facility-based environment, it can be easily applied in any environment due to its convenience, making it especially useful in low-resourced countries 4.
Surprisingly, the KMC, a medical innovation with many benefits, is globally underutilised 5. Increasing the practice thereof, especially in low- to lower-middle- income environments, may decrease the rates of neonatal mortality.
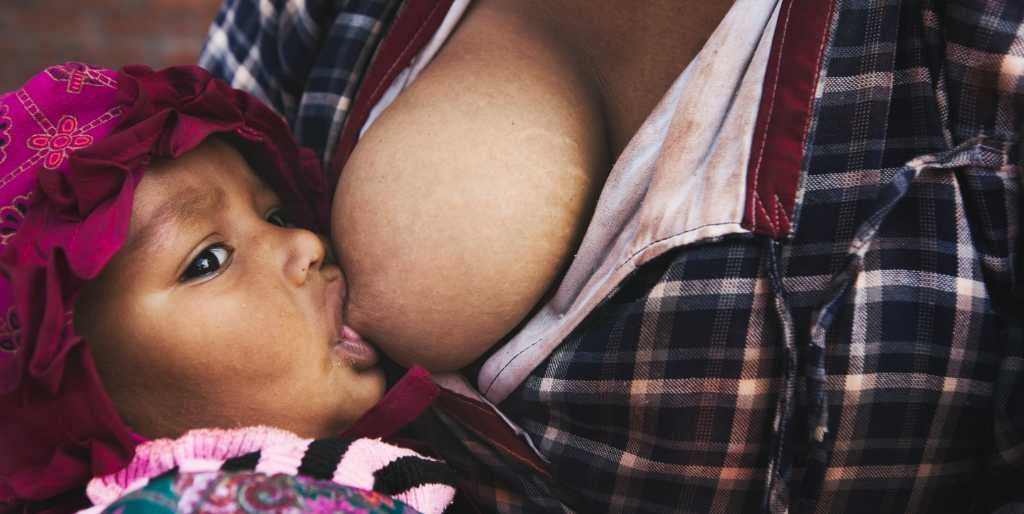
Breastfeeding
Breastfeeding offers benefits for both the mother and baby. Infants receive nutrition (which is especially important for under-weight and/or premature infants), immunisation, developmental benefits, as well as long term benefits such as increased IQ scores and reduced risk of becoming overweight or developing diabetes 5,6. Breastfeeding mothers receive protection from breast and ovarian cancer, as well as type 2 diabetes. Additionally, breastfeeding can improve birth spacing 6.
Research has shown the importance of initiating breastfeeding within the first hour after birth, this builds good health and reduces the risk for infection, thus neonatal mortality rates 5,14. For pre-term infants, breastfeeding is considered optimal because of its short-term and long-term benefits in comparison to formula feeding. This includes reduced infection rates, a reduced risk of necrotising enterocolitis and improved neurodevelopment 5. This makes breastfeeding a valuable ally in boosting health and wellness in both mother and child, and thus should be recommended in low- and lower-middle- income countries.
Nutrition Education
Studies have indicated that most women in developing countries do not consume adequate nutrients in line with the Recommended Dietary Allowance 7. In addition to this, they continue to endure heavy physical activity during their pregnancies, thus increasing their nutritional requirements further 7. These women tend to not gain sufficient weight during pregnancy and may become malnourished. In turn, this increases the risk of miscarriage, stillbirth, preterm or low-weight infants, neonatal death, birth defects, cretinism, reduced IQ, infections, anaemia and maternal mortality 7.
Nutritional education and counselling are seen as vital interventions to optimise maternal nutrition and thus improve pregnancy outcomes 7. An alteration of positive behaviour has been recorded by research from many authors on participants who received this service 7. It is therefore recommended that governments include these services in primary healthcare arrangements for pregnant women 7. Studies in Uganda, Malawi and Ethiopia, for instance, found that nutrition education for caregivers lead to better food choices and an increase of meals with a higher quality 10,12,13.
The following are examples of tools and services for HCPs to make use of when educating those in low-resource and developing countries:
- Educational material

Excerpt of the Infant and Young Child Feeding cards by UNICEF 8.
Above is an extraction of the Infant and Young Child Feeding cards. These cards have been created by United Nations Children’s Fund (UNICEF) New York, Nutrition Policy Practice (NPP) and the Centre for Human Services, the not-for-profit affiliate of University Research Co., LLC (URC/CHS) 8.
Uganda has made these counselling cards a standard practice in their health sector to educate caregivers on childcare and feeding. Nutrition education cards have been shown to boost infant and young child nutrition as well as growth patterns in Uganda 8,10. It is suggested that other countries, especially low-resourced countries, should make use of nutrition education cards to experience the same benefits as the East and Southern Africa Region countries mentioned above. These cards are useful as they are easy to understand and access or distribute, if printed.
Furthermore, the World Health Organisation and UNICEF compiled Infant and Young Child Feeding counselling cards in the context of COVID-19. These cards have the purpose of promoting hygiene precautions to assist families and communities in preventing the spread of the virus 11.
- Strategies to improve maternal nutrition
|
Tips that HCPs can give to mothers |
|
|
|
|
Table to be used by HCPs to advise adequate nutrition intake 7, 9.
Conclusion
In low-income and under-resourced countries, the relatively high prevalence of premature births presents a considerable challenge for HCPs. Simple, cost-effective interventions and tools, some as simple as the holding of baby to its mother’s chest, could have significant impact.
References:
- Bantham, B. 2020. World Prematurity Day 2020- turn awareness into action. https://news.nwu.ac.za/world-prematurity-day-2020-%25E2%2580%2593-turn-… Date of access: 17 Nov. 2021.
- Howson, CP., Kinney, MV. and Lawn, JE. 2012. Born Too Soon: The Global Action Report on Preterm Birth. World Health Organization: Geneva.
- World Health Organization, 2019. Estimates Developed by the UN Inter-Agency-Group for Child Mortality Estimation. https://www.unicef.org/reports/levels-and-trends-child-mortality-report-2020 Date of access: 11 Nov. 2021.
- Hailegebriel, T.D., Bergh, A.M., Zaka, N., Roh, J.M., Gohar, F., Rizwan, S., Asfaw, A.G., Heidarzadeh, M. and Zeck, W., 2021. Improving the implementation of kangaroo mother care. Bulletin of the World Health Organization, 99(1), p.69. doi: 10.2471/BLT.20.252361
- Lawn, J.E., Davidge, R., Paul, V.K., von Xylander, S., de Graft Johnson, J., Costello, A., Kinney, M.V., Segre, J. and Molyneux, L., 2013. Born too soon: care for the preterm baby. Reproductive health, 10(1), pp.1-19. doi: 10.1186/1742-4755-10-S1-S5
- Victora, C.G., Bahl, R., Barros, A.J., França, G.V., Horton, S., Krasevec, J., Murch, S., Sankar, M.J., Walker, N., Rollins, N.C. and Group, T.L.B.S., 2016. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. The Lancet, 387(10017), pp.475-490. doi: 10.1016/S0140-6736(15)01024-7
- Odiwuor, F., 2020. Nutrition education and counselling: an essential consideration to optimise maternal nutrition and pregnancy outcomes in Kenya.
- UNICEF. s.a. Infant and young child feeding: counselling cards for community workers. https://www.unicef.org/media/108406/file/Counselling%20Cards.pdf Date of access: 15 Nov. 2021.
- Gernand, A.D., Schulze, K.J., Stewart, C.P., West, K.P. and Christian, P., 2016. Micronutrient deficiencies in pregnancy worldwide: health effects and prevention. Nature Reviews Endocrinology, 12(5), pp.274-289.
- MK, K. and Bonsi, E.A., 2021. Improving caregivers' infant and young child-feeding practices using a three-group food guide: a randomized intervention study in central Uganda. African Journal of Food, Agriculture, Nutrition & Development, 21(4).
- USAID. s.a. Infant and young child feeding recommendations when COVID-19 is suspected or confirmed. https://www.advancingnutrition.org/what-we-do/social-and-behavior-change/iycf-recommendations-covid-19#design-files Date of access: 17 Nov. 2021.
- Katenga-Kaunda, L.Z., Iversen, P.O., Holmboe-Ottesen, G., Fjeld, H., Mdala, I. and Kamudoni, P.R., 2020. Dietary intake and processes of behaviour change in a nutrition education intervention for pregnant women in rural Malawi: a cluster-randomised controlled trial. Public Health Nutrition, 23(13), pp.2345-2354.
- Demilew, Y.M., Alene, G.D. and Belachew, T., 2020. Effect of guided counseling on dietary practices of pregnant women in west Gojjam zone, Ethiopia. Plos one, 15(5), p.e0233429.
- Nestle Nutrition Institute. 2021. Breastfeeding: protecting the golden hour. https://nnia.nestlenutrition-institute.org/news/article/2021/08/18/brea… Date of access: 17 Nov. 2021.
If you liked this post you may also like



